- 2nd Floor, Shaligram Lakeview Commercial, nr. Vaishnodevi Circle, Ahmedabad
Keratoconus Treatment in Ahmedabad
Keratoconus is one of the most common progressive corneal conditions, yet it is frequently misdiagnosed as high astigmatism in its early stages. If you or someone in your family has been experiencing worsening vision despite regular changes in glasses, or a prescription that does not seem to fully correct your sight, a comprehensive corneal evaluation at Krisha Eye Hospital in Ahmedabad can provide a clear diagnosis and a treatment plan built around your specific stage of the condition.
What is Keratoconus?
Keratoconus is a progressive condition of the cornea, the clear front surface of the eye, in which the normally dome-shaped cornea gradually thins and begins to bulge forward into an irregular, cone-like shape. As the cornea loses its normal curvature, it can no longer focus light accurately onto the retina, resulting in blurred and distorted vision that cannot be fully corrected with standard spectacles.
The condition typically begins during the teenage years or early twenties and may progress slowly over one to two decades before stabilising on its own. It affects both eyes in the majority of cases, though the severity is often quite different in each eye. The exact cause is not fully understood, but a combination of genetic predisposition and environmental factors, including habitual eye rubbing, is thought to play a significant role.
Diagnosis requires corneal topography or tomography, which maps the shape and thickness of the cornea in detail. Standard sight tests and retinoscopy alone are not sufficient to detect keratoconus reliably. If you are experiencing unusual or rapidly changing vision, a comprehensive eye examination in Ahmedabad is the right first step before any treatment decisions are made.
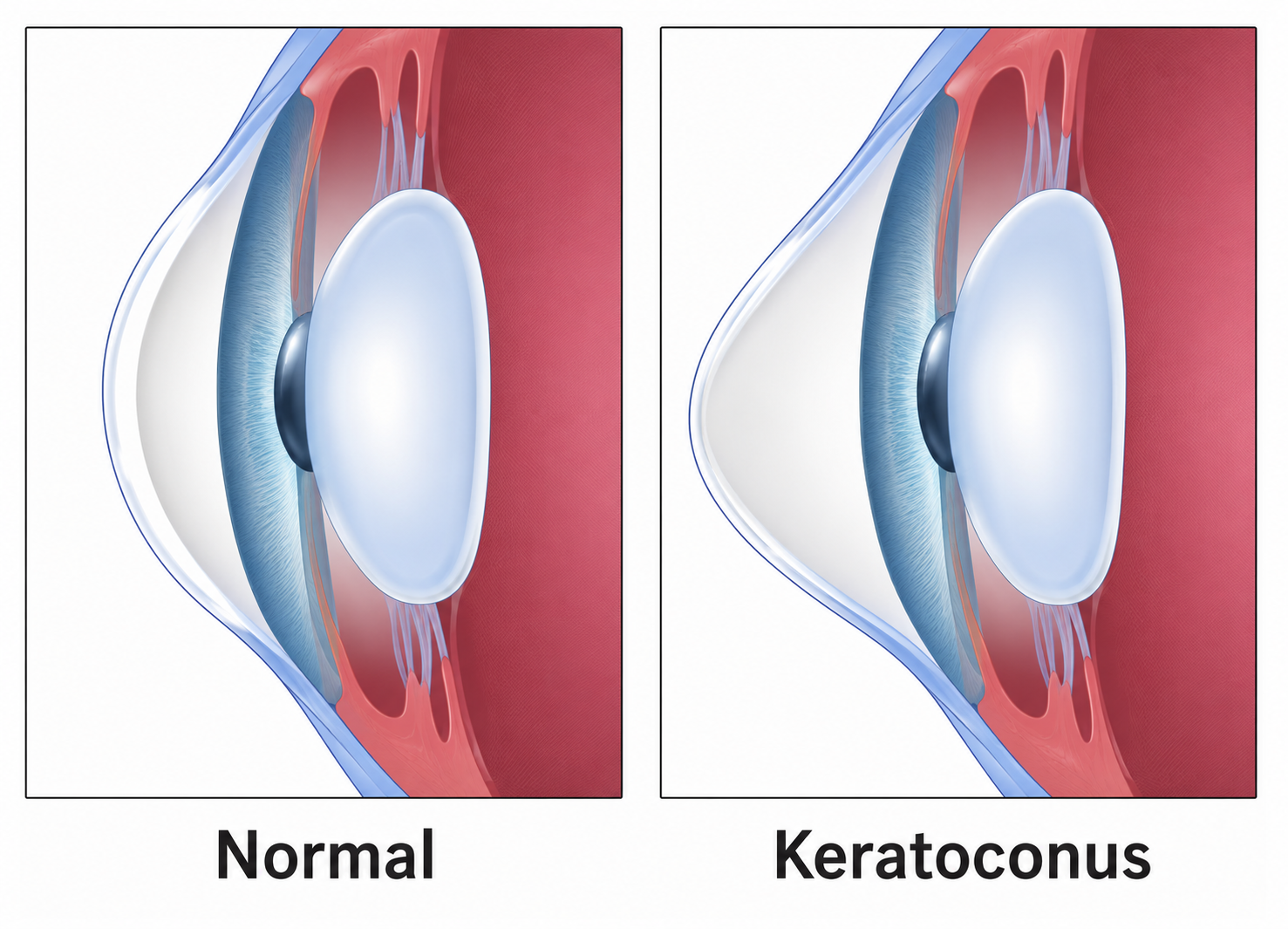
Keratoconus presents differently depending on the stage of the condition. In the early stages, symptoms are often subtle and easy to dismiss as ordinary vision changes. As the condition advances, vision disturbances become more pronounced and begin to affect daily activities. Understanding the full picture helps your doctor identify the right point in time for treatment.
Use the tabs below to explore symptoms, causes, and what can happen if keratoconus is not diagnosed and managed in time.
Common Symptoms of Keratoconus
- Blurred or distorted vision that spectacles do not fully correct
- Increased sensitivity to light and glare, particularly when driving at night
- Frequent and unexplained changes in spectacle prescription over a short period
- Ghosting or double vision in one eye when the other eye is closed
- Difficulty with tasks requiring sharp detail, such as reading small text or recognising faces at a distance
- Halos and streaking around light sources after dark
- Eye strain and visual fatigue after short periods of concentration
Causes and Risk Factors for Keratoconus
- Genetic predisposition; having a first-degree relative with keratoconus significantly increases personal risk
- Chronic and vigorous eye rubbing, which physically degrades the corneal collagen structure over time
- Atopic conditions including hay fever, eczema, and allergic asthma, which lead to frequent eye rubbing
- Down syndrome and connective tissue disorders such as Marfan syndrome and Ehlers-Danlos syndrome
- South Asian populations have a higher recorded prevalence compared to Western populations
- Prolonged UV light exposure without adequate eye protection
Complications of Untreated or Unmonitored Keratoconus
- Progressive worsening of vision that can no longer be corrected by spectacles as the cornea becomes more irregular
- Acute corneal hydrops: a sudden swelling of the cornea caused by a break in Descemet's membrane, resulting in rapid vision loss and pain requiring urgent care
- Corneal scarring in advanced stages, which can permanently reduce vision quality
- Inability to tolerate contact lenses as the cone shape becomes too extreme
- Need for corneal transplant surgery in severe or end-stage cases where no other option remains
Grades of Keratoconus
Keratoconus is not a single fixed condition. It progresses through identifiable stages, and the grade at diagnosis directly determines which treatments are appropriate and how urgently they need to be initiated.
Subclinical Keratoconus
Also referred to as forme fruste keratoconus, this is the earliest detectable stage. The cornea shows subtle shape changes on topography mapping but vision is not yet affected and the eye appears normal on standard examination. Identification at this stage is critical because subclinical keratoconus is a contraindication to LASIK and similar refractive procedures.
Mild Keratoconus
Vision can still be corrected reasonably well with spectacles or soft contact lenses, though the correction may not be as sharp as expected. The corneal irregularity is present but limited. Corneal cross-linking at this stage provides the best opportunity to halt progression before significant vision loss develops.
Moderate Keratoconus
Standard spectacles are no longer adequate for clear vision. Rigid gas permeable or scleral contact lenses become necessary. Cross-linking is still effective at this stage. Intrastromal ring segment implantation may be considered alongside cross-linking to improve contact lens fit and tolerance.
Advanced and Severe Keratoconus
The cornea has a pronounced cone shape, often with visible thinning and sometimes scarring at the apex. Contact lens wear becomes very difficult or impossible. If usable vision cannot be achieved through lenses alone, corneal transplant surgery may be the only remaining option to restore functional sight.
Treatment Options for Keratoconus in Ahmedabad
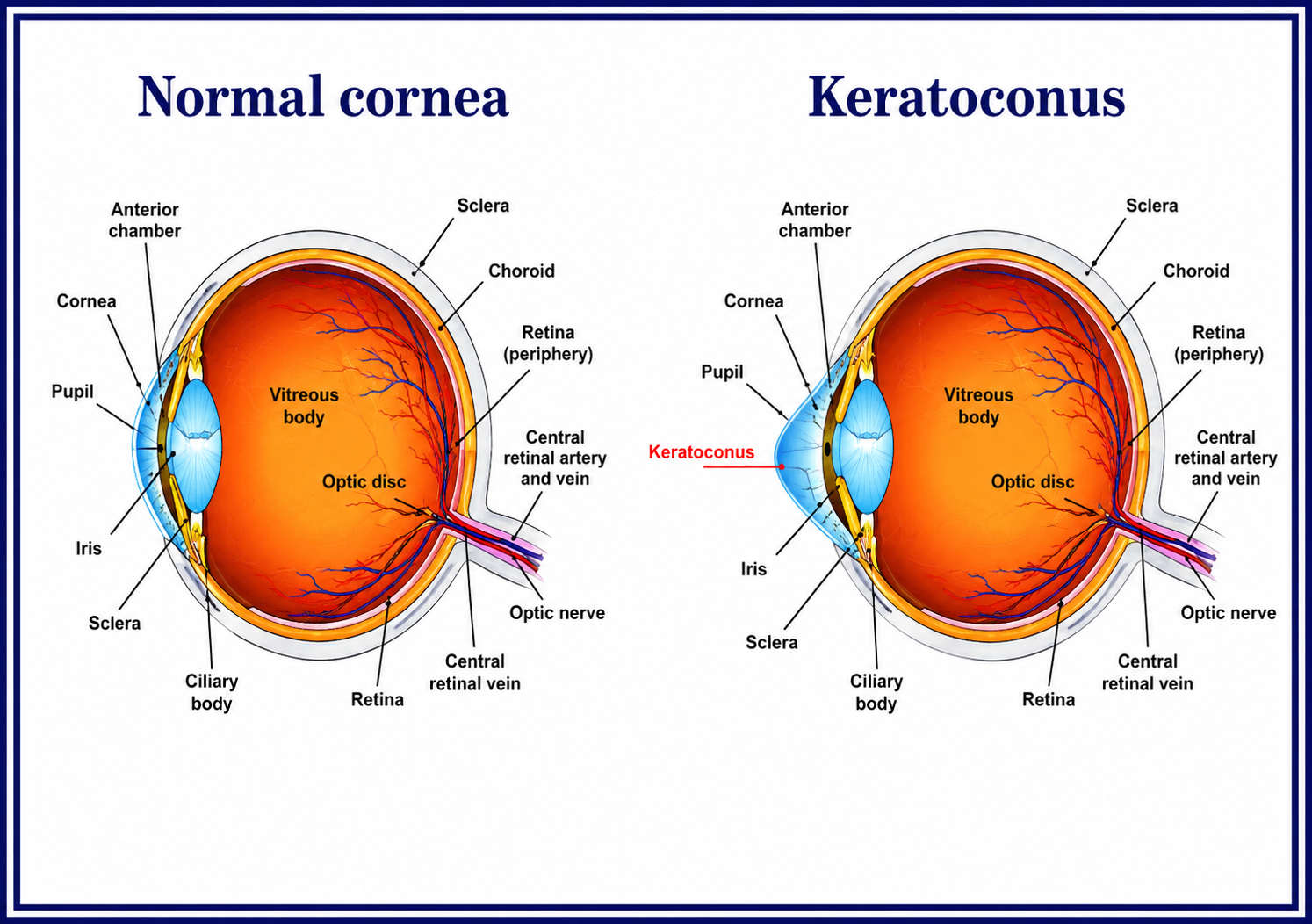
The right treatment for keratoconus depends entirely on the grade of the condition, the rate of progression, the current level of vision, and how well contact lenses are tolerated. At Krisha Eye Hospital, we assess each patient thoroughly before recommending any intervention. For many patients, a combination of approaches is used at different stages.
Spectacles and Soft Contact Lenses
Effective in the early stages when the corneal irregularity is still mild. As the condition progresses, the irregular corneal surface can no longer be corrected adequately by standard lenses. Early-stage patients on spectacles should be monitored closely with regular topography to detect any progression promptly.
Rigid Gas Permeable (RGP) Contact Lenses
RGP lenses vault over the irregular corneal surface and replace it optically with a smooth, uniform refracting surface, providing significantly better vision than spectacles. They are the standard optical correction for mild to moderate keratoconus and are well tolerated by most patients with careful fitting and ongoing follow-up.
Scleral Contact Lenses
Larger than standard RGP lenses, scleral lenses rest on the white of the eye rather than directly on the cornea. They are filled with preservative-free saline before insertion, creating a smooth liquid layer over the corneal surface. Particularly useful for advanced keratoconus and for patients who cannot comfortably tolerate smaller RGP lenses.
Corneal Cross-Linking (C3R / CXL)
Corneal cross-linking is the most important treatment for halting the progression of keratoconus. It uses riboflavin (vitamin B2) eye drops combined with controlled UV-A light to strengthen the collagen fibres within the cornea, making it more resistant to further bulging. C3R does not reverse the existing cone shape, but it stops or significantly slows further progression. It is most effective when performed during the mild to moderate stage before significant vision loss has occurred.
Intrastromal Corneal Ring Segments (ICRS)
Thin, curved arc-shaped implants placed within the corneal stroma to flatten and regularise the cone. They can improve contact lens tolerance and, in suitable cases, reduce the degree of optical correction required. Often combined with cross-linking. Not appropriate for corneas with central scarring or very advanced disease.
Corneal Transplant (DALK / PKP)
Reserved for advanced cases where vision cannot be adequately corrected through contact lenses, or where significant scarring is present. Deep Anterior Lamellar Keratoplasty (DALK) is now preferred over full-thickness penetrating keratoplasty (PKP) in most keratoconus cases, as it preserves the patient's own inner corneal layer and carries a lower long-term rejection risk. Our cornea specialists in Ahmedabad assess each case individually before recommending surgery.
Before, During and After Your Appointment
Before Your Appointment
Attend your consultation with a note of when you first noticed changes in your vision, and bring your current spectacle prescription if you have one. Avoid wearing contact lenses for at least 24 to 48 hours before a corneal topography assessment, as lens wear can temporarily change the shape of the cornea and affect the accuracy of the map. If you are being evaluated for suitability for cross-linking, your doctor will review both your topography maps and corneal thickness measurements before confirming whether the procedure is appropriate for you.
During Your Appointment
Corneal topography is a quick, non-invasive scan completed in the clinic. For corneal cross-linking, the procedure is performed under topical anaesthetic drops and takes approximately 30 to 60 minutes depending on the protocol used. The procedure involves applying riboflavin drops to the cornea at regular intervals before controlled UV-A light exposure. There is no pain during the procedure itself. For contact lens fitting, the corneal map is used to select and trial an appropriate lens design before a final fitting is confirmed.
After Your Appointment
After cross-linking, a bandage contact lens is typically placed on the eye for the first few days to protect the corneal surface while it heals. Mild discomfort, light sensitivity, and temporary blurring are expected in the first one to two weeks. Corneal topography maps are reviewed at three months, six months, and then annually to confirm that progression has been halted. It is important to understand that the goal of cross-linking is stabilisation, not vision improvement. Vision correction is then addressed separately through spectacles or contact lenses.
Why Choose Krisha Eye Hospital for Keratoconus Treatment?
- Corneal topography assessment to accurately grade the stage of keratoconus before any treatment is recommended
- Corneal cross-linking (C3R) available for eligible patients to halt disease progression
- Expert contact lens fitting for RGP and scleral lenses, with ongoing follow-up and lens adjustments
- Surgical options including ICRS and corneal transplant (DALK and PKP) discussed transparently based on individual suitability
- No unnecessary interventions: if observation and monitoring is the most appropriate plan at your stage, that is what we recommend
- All assessments include a clear explanation of findings, the grade of your condition, and the proposed management approach
- Convenient location near Vaishnodevi Circle, Ahmedabad
Can Keratoconus Be Managed?
Keratoconus cannot be prevented, as the underlying genetic predisposition cannot be changed. However, certain habits and proactive steps can significantly reduce the risk of rapid progression and help protect the vision you have.
- Stop rubbing your eyes. This is the single most important change you can make. Habitual eye rubbing degrades the corneal collagen structure and is one of the strongest known modifiable risk factors for progression. If your eyes itch, use cold compresses or antihistamine drops rather than rubbing.
- Treat underlying allergies. Uncontrolled hay fever or allergic conjunctivitis leads to persistent eye irritation and the urge to rub. Proper allergy management, with antihistamine drops or systemic treatment, reduces this risk significantly.
- Attend regular corneal topography reviews. If you are in a progressive phase of the condition, six-monthly topography maps are the minimum requirement. Early detection of progression allows cross-linking to be performed before significant vision loss occurs.
- Wear UV-protective sunglasses outdoors. UV light is thought to contribute to oxidative stress in the cornea. Good-quality wraparound sunglasses offer practical protection.
- Arrange screening if you have a family history. First-degree relatives of keratoconus patients have a significantly higher risk. A corneal topography scan can detect subclinical changes before symptoms appear and before any irreversible refractive procedure is considered.
What Our Patients Say
These are real experiences shared by patients who came to Krisha Eye Hospital for keratoconus treatment in Ahmedabad.
Rohan Mehta
Software Developer, Ahmedabad
"I had been changing my glasses prescription every eight to ten months for three years and never understood why my vision was not fully improving. My optician always said it was just astigmatism. When I finally came to Krisha Eye Hospital, the doctor did a corneal topography scan during the first visit and explained clearly that I had keratoconus in both eyes, the right being more advanced. She went through the whole condition, what it meant, and what my options were. I had C3R cross-linking done on both eyes in two separate sessions. The procedure was not painful and recovery was straightforward. Seven months on, my last topography scan showed no progression. I am now wearing scleral contact lenses and my vision is better than it has been in years. I only wish I had come sooner."
★★★★★
Prachi Joshi
Student, Ahmedabad
"I was 17 when my parents noticed I was squinting and struggling to see the board at school even with my glasses on. A previous doctor had given me stronger glasses twice in the same year but never mentioned keratoconus. At Krisha Eye Hospital, the first thing they did was a proper corneal scan. The doctor diagnosed early keratoconus and explained that we had caught it at a good stage. She recommended cross-linking as soon as possible to prevent it from getting worse. I was nervous about any procedure near my eyes but the team was very patient and explained every step before doing it. The procedure took about 45 minutes and I was back at school within a week. My scans since then have been completely stable. I am now in my second year of college wearing RGP lenses and managing perfectly well."
★★★★★
Haresh Patel
Businessman, Ahmedabad
"I had visited two other hospitals before coming to Krisha Eye Hospital and both told me I would need a corneal transplant fairly soon. I was understandably worried and came here for a second opinion. The doctor reviewed my topography maps carefully and explained that while my keratoconus was at an advanced stage, my corneal thickness was still within the range suitable for cross-linking and there was no scarring that would make transplant immediately necessary. She was very direct about what the procedure could and could not achieve. I had cross-linking done and was fitted with scleral lenses, which have genuinely changed my daily life. I can work, read, and drive again without constant visual difficulty. I am still on regular monitoring but the transplant has not been needed. I was given an honest assessment rather than an alarming one."
★★★★★
Sunita Parmar
School Teacher, Ahmedabad
"My daughter was diagnosed with keratoconus at 19 after several years of what we assumed was just poor eyesight. When she was confirmed to have it, I came to Krisha Eye Hospital to get myself checked as well, since I had been told there is a family link to the condition. The doctor found early topographic changes in my cornea that were not yet affecting my vision in any noticeable way. I am now on six-monthly monitoring visits with repeat corneal maps each time. No treatment has been needed beyond observation and my current glasses, which is reassuring. What I value most is that the doctor is always honest about where I stand and does not recommend intervention unless it is genuinely indicated. I feel properly looked after."
★★★★★
Our Doctor
Questions about keratoconus are best answered in person with a full corneal assessment. Dr. Dhwani Maheshwari and the team at Krisha Eye Hospital assess each patient carefully before any treatment recommendation is made.

Dr. Dhwani Maheshwari
Cataract & Refractive Surgeon | Krisha Eye Hospital, Ahmedabad
Dr. Dhwani Maheshwari completed her DOMS from Civil Hospital Ahmedabad and has performed more than 5,000 eye surgeries. She leads comprehensive eye care at Krisha Eye Hospital, including the diagnosis and management of corneal conditions such as keratoconus. Her approach begins with accurate grading of the condition, followed by a treatment plan that is matched to what each patient actually needs at their current stage.
Book ConsultationFrequently Asked Questions
Is keratoconus curable?
There is no treatment that reverses the change in corneal shape already caused by keratoconus. However, corneal cross-linking (C3R) can halt or significantly slow further progression, and with appropriate optical correction through RGP or scleral contact lenses, most patients maintain good functional vision for many years. In severe cases where vision can no longer be corrected adequately, corneal transplant surgery can restore useful sight. The key is early diagnosis and timely management before significant vision loss develops.
At what age does keratoconus typically begin?
Keratoconus most commonly begins during the teenage years or early twenties, though it has been diagnosed in younger children and in adults in their thirties. Progression tends to be most rapid in younger patients and generally stabilises naturally in the mid to late thirties. This is precisely why early treatment with cross-linking, when indicated, matters: performing the procedure while the cornea still has adequate thickness and before significant vision loss occurs gives the best long-term outcome.
What is C3R and is it painful?
C3R stands for Collagen Cross-Linking of the Cornea using Riboflavin, which is the term commonly used in India for corneal cross-linking. The procedure involves applying riboflavin (vitamin B2) drops to the cornea and then exposing it to controlled UV-A light to strengthen the collagen bonds and slow progression. It is performed under topical anaesthetic drops and is not painful during the procedure itself. In the days following treatment, some discomfort, watering, and light sensitivity are expected while the corneal surface recovers. Most patients return to normal activity within one to two weeks.
Can I wear contact lenses if I have keratoconus?
Yes, in most cases. Rigid gas permeable (RGP) and scleral contact lenses are the primary means of achieving good vision in keratoconus that cannot be corrected well enough by spectacles. Scleral lenses in particular provide excellent visual clarity for irregular corneas by creating a smooth liquid layer over the corneal surface. The lens design needs to be tailored carefully to the shape of your individual cornea, which requires specialist fitting and follow-up. Our cornea and contact lens team in Ahmedabad handles this as part of ongoing keratoconus management.
How will I know if my keratoconus is getting worse?
Progression is confirmed through serial corneal topography. If your maps show an increase in corneal curvature or a reduction in corneal thickness over time, your keratoconus is considered progressive. Subjective indicators such as worsening vision, the need for a stronger prescription, or increasing difficulty tolerating your contact lenses can also suggest progression, but topography is the definitive measure. Regular check-up appointments, at least every six months if you are in an active phase, are essential to detect any change before it becomes significant.
What is the cost of keratoconus treatment in Ahmedabad?
The cost depends entirely on the treatment required, which is determined by your grade of keratoconus, the rate of progression, and your vision correction needs. A consultation and corneal topography assessment are charged separately from any procedure. Cross-linking, scleral lens fitting, ICRS implantation, and surgical options each carry different costs. Krisha Eye Hospital provides a clear and complete cost breakdown during your first consultation so there are no surprises. Contact us to arrange an assessment.
Does keratoconus affect both eyes?
Keratoconus is a bilateral condition in the majority of cases, meaning it affects both eyes. However, it is rarely symmetrical. One eye is typically more advanced than the other, and in some patients the second eye shows only very mild topographic changes with no meaningful effect on vision. Both eyes should be assessed and monitored at every visit, even when one eye appears to be completely stable. Treatment decisions are made separately for each eye based on the individual topography findings.
Concerned About Your Vision or a Keratoconus Diagnosis?
Book a corneal assessment at Krisha Eye Hospital, Ahmedabad. Get an accurate grading of your condition and a treatment plan matched to your specific stage.
2nd Floor, Shaligram Lakeview Commercial, near Vaishnodevi Circle, Ahmedabad 382421 | +91 75677 67701
Related Treatments at Krisha Eye Hospital
Explore other services offered by our team in Ahmedabad.
Contact Us For Any Further Question
Address 2nd Floor, Shaligram Lakeview Commercial, near Vaishnodevi Circle, Ahmedabad 382421
Phone +91 75677 67701
Hours Mon–Sat: 10:30 AM – 1:30 PM & 6:00 PM – 7:30 PM
Medical Disclaimer: The information on this page is provided for general educational purposes only and does not constitute medical advice. It is not a substitute for a professional consultation, diagnosis, or treatment by a qualified eye care specialist. If you are experiencing eye symptoms, please contact a doctor. Krisha Eye Hospital, Ahmedabad.
